
Answering your most-asked menopause questions
1. What is Menopause?
You are in menopause when you have not had a period for 12 months. Thereafter, you are officially post-menopause. The transition from regular, cyclic reproductive cycles to never ovulating again (menopause) is called perimenopause. The perimenopause transition lasts somewhere between 4-10 years for most women.
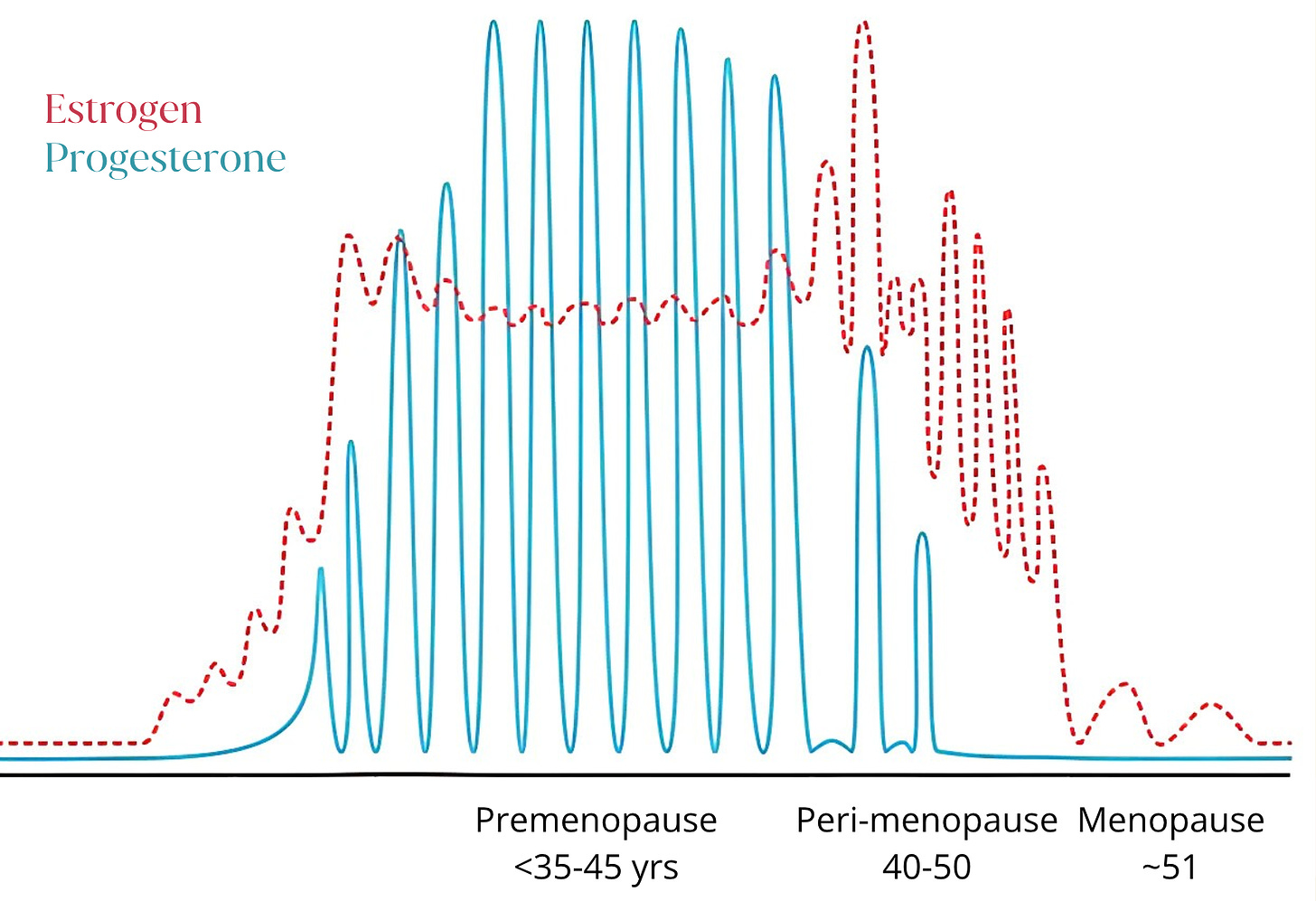
This graph tells the story of how our main reproductive hormones, estrogen and progesterone, fluctuate wildly during the perimenopause transition. At the beginning of perimenopause, estrogen levels can be high: your body is trying to rev up its ovulation in protest! And, in comparison, progesterone levels are decreasing.
Higher estrogen leads to:
• Heavy menstrual cycles - which can start to get closer together
• Breast tenderness
• Fibroid formation
Decreasing progesterone leads to:
• Longer periods
• PMS, PMDD symptoms
• Poor sleep
• Anxiety
Your menstrual cycle ultimately starts to slow down and ovulation becomes more and more sporadic. Estrogen and progesterone levels drop, causing our periods to space out and also bringing on the classic symptoms of low estrogen.
2. What are the key symptoms associated with menopause?
While many of us associate menopause with the classic “vasomotor” symptoms of hot flashes and night sweats, the menopause transition actually includes over 30 symptoms. We have estrogen receptors all over our body. As estrogen drops, symptoms can show up almost anywhere - even in our inner ears.
This body map marks some of the common menopause symptoms:
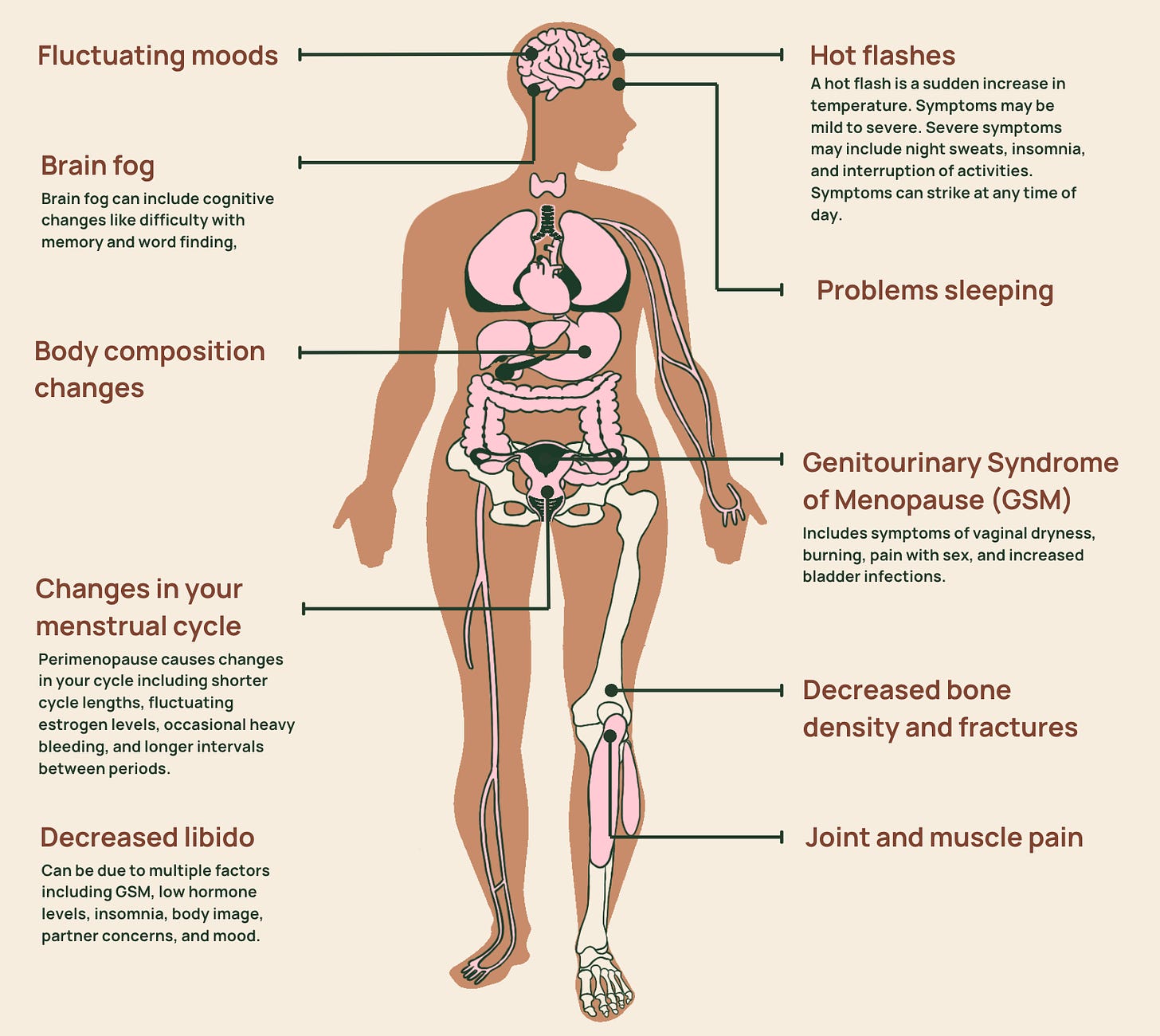
Note: Black and Hispanic women are at particularly high risk for severe vasomotor symptoms.
3. What are treatments for menopause transition symptoms?
HORMONAL TREATMENTS
1. Hormonal contraceptives:
These provide management for both symptoms during perimenopause AND contraceptive protection. This is a good thing! Contraceptives can be combined estrogen/progesterone or progesterone only. Moreover, contraceptives are often a better choice in early perimenopause for women struggling with heavy, unpredictable periods
2. Menopausal Hormone Therapy (MHT), also known as “HRT”:
A) SYSTEMIC estrogen: Circulates in bloodstream.
Consists of a lower dose (than contraceptive pills) of estrogen +/- progesterone (if you have a uterus).
Considered first-line treatment for:
• Hot flashes/night sweats
• Early Menopause (age <45), and Primary Ovarian Insufficiency (menopause <40)
• Prevention of osteoporosis
B) LOCAL estrogen: Applied directly to the vagina.
Stays at the local tissue level and is not absorbed into the bloodstream.
Helps with:
• Vaginal Dryness and other GSM-related* changes
*Genitourinary syndrome
NON-HORMONAL TREATMENTS
Hormone therapy is not the only option available. There are non-hormonal medications including Gabapentin, two classes of medications typically used for mood/anxiety symptoms (SSRIs and SNRIs2 ). As well, a new medication will be coming out in early 2025 which acts directly on the temperature centre of the brain (we are very excited about this one!)
NON-PHARMACOLOGICAL TREATMENTS
Cognitive behaviour therapy, weight loss and clinical hypnosis have also shown improvement in vasomotor symptoms. While not specific to menopausal symptoms, ensuring good nutrition, adequate sleep, exercise, and strong relationships lays the foundation for our well-being.
4. Is there anything else hormone therapy (MHT) may be helpful for?
• Hormone therapy may be beneficial to treat mood changes including depression and anxiety during the menopause transition. Women who experienced mood changes with periods or after having a baby seem to benefit the most.
• Hormone therapy may also help women who are struggling with joint pains and body aches related to the menopause transition.
• There has been a lot of attention around the use of hormone therapy as a prevention strategy in terms of heart disease, dementia and longevity. While there is encouraging research on the benefits of hormone therapy, it is not a panacea for ageing well and more research is needed.
Sources
• The musculoskeletal syndrome of menopause
• The Menopause Society 2024 Survey